
Choosing Your Local Anaesthetic
Options to Manage Young Patients' Pain
This is the first in a series of articles on local anaesthetic designed to assist the reader in local anaesthetic usage.
This first article explores the chemical properties of local anaesthetic and how these properties could determine which local anaesthetic is best suited for the patient and the procedure. From the outset, it should be recognised local anaesthetics are inherently safe with very side effects and a long history of safety. While many dentists use a particular local anaesthetic because they have always used it and it works in their hands; practitioners should not be blinded to the fact that there may be a better solution with increased efficacy and safety.
What outcomes should a local anaesthetic have?
There are 4 outcomes that the dentist requires of their local anaesthetic:
1. That it works quickly, so as to efficiently use the time available for treatment.
2. That the analgesia is profound enough to allow the procedure to be pain free.
3. That is duration of action is long enough to complete the task and,
4. That it is safe, for that patient.
What determines these outcomes for local anaesthetic? It Works quickly.
The most important factor that determines the onset of anaesthesia is the proportion of the local anaesthetic molecules that exist in a lipid-soluble rather than a water-soluble state [1]. The local anaesthetic within the cartridge is an acidic solution with a pH ~ 4 but once it is injected into the extracellular tissue it rapidly reaches the psychological pH 7.4. During this process molecule changes from the ionised form to the non-ionised form which is lipid soluble.
The equation which determines the rate at which the molecules are de-ionised and re-ionised is known as the Henderson-Hasselbalch Equation:
pKa = pH + log [AH]/[A-]
The equation shows the relationship between the pKa and pH to the bioavailability of active ions to bind to the receptor sites and hence block the nerve channel. The pKa is the pH at which a weak acid or weak base will be 50% ionised 2.1 To summarise what this means;
The closer the pKa is to the physiological pH the quicker the onset.
Profoundness
How profound a local anaesthetic solution is largely determined by its lipid solubility. The lipid solubility of a local anaesthetic is important as the nerve membrane is a lipid environment. It is the aromatic group of the local anaesthetic which gives it lipid solubility. An increase in lipid solubility will lead to more local anaesthetic passing through the nerve walls to act on the binding site. Greater lipid solubility of a drug not only enhances potency but also enables more rapid diffusion through cell membranes. However, if it is too lipid soluble, it may impede dispersion throughout tissue fluids and foster sequestration in neighbouring adipose tissues or myelin sheaths.
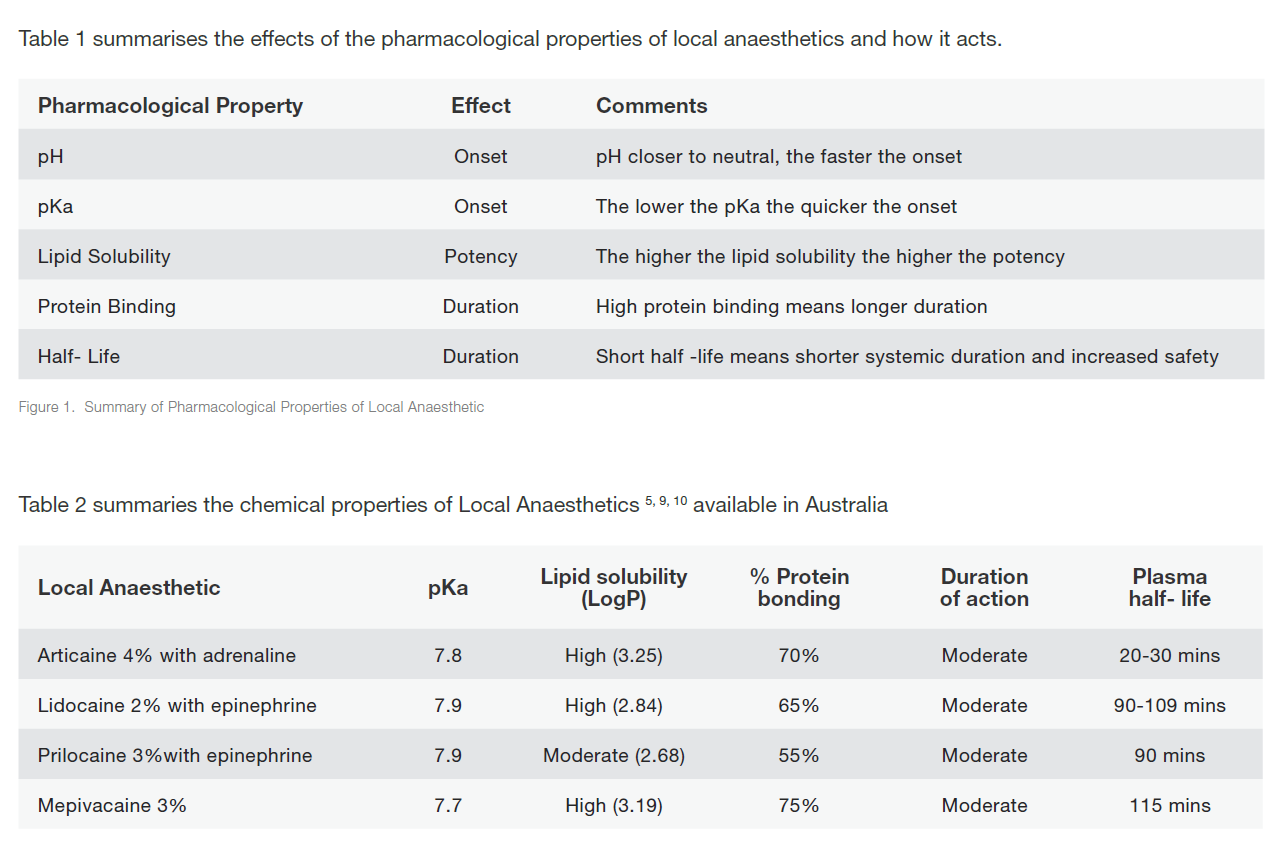
A measure of a local anaesthetic is the LogP value, where the ideal local anaesthetic should have a value between 2-4. Small differences in the LogP will equate to a large difference in the actual number of ions available e.g. Articaine's log P is 3.25 while Lignocaine is 2.84 which means that Articaine is four times more lipid soluble.
The receptor sites in the sodium channels are protein rich and local anaesthetics will vary in their duration of action due primarily to differences in their ability to bind to those protein sites and the percentage of circulating local anaesthetic that is protein bound has been found to correlate with an anaesthetic's affinity for protein within sodium channels. Furthermore, the percentage of unbound local anaesthetic in the blood/plasma is an important consideration in toxicity. The greater the local anaesthetic protein binds, the longer the local anaesthetic duration of action [3].
Safety
A drug's half- life is the time needed to achieve a 50% reduction in anaesthetic in the blood levels and it takes 4 Half-Life's for a drug to be considered cleared from the system (94% is eliminated) [4]. A short half-life means a shorter duration in the blood stream and important consideration with toxicity, re- injection and safety.
All amide local anesthetics are metabolized in the liver to varying degrees. Lignocaine is almost entirely metabolized by the liver by a variety of enzymes to numerous metabolites. Approximately 90% of Lignocaine administered is excreted in the form of various metabolites, and less than 10% is excreted unchanged. Prilocaine is metabolised in both the liver and the kidney and like Lignocaine is mainly metabolised by the liver [5]. Mepivacaine, while it too, is metabolised by the liver, 50% of the metabolites are excreted into the bile.
With Articaine, while it has the basic structure of an amide based local anaesthetic, it has an additional ester component. Therefore, it is 95% metabolised by the cholinesterase in the plasma producing an inert metabolite of articainic acid which is excreted via the kidneys, Therefore it is half-life is considerably shorter than other amide based local anaesthetics [6].

Additional Factors
Adrenaline is often added to local anaesthetic preparations for 4 reasons which relate to its vasoconstrictive and systemic properties:
- It increases the amounts of local anesthetic that remain in and around the nerve for longer periods and hence increases duration.
- It will also decrease bleeding at the site of administration, and
- By decreasing the spread of local anaesthetic from the site of administration, it decreases the amount of systemic local anaesthetic, and therefore its toxicity.
- Used as a marker for intravascular injection. An intravascular injection of adrenaline will cause a short-lived increase in heart rate, notifying the dentist of a potential toxicity issue [7].
It does, however, have some unwanted side effects due to adverse reactions with medications, cardiovascular disease and peripheral ischemia [8].
Author: Dr Greg Mahoney
BDSc, PhD, MSc(Dent), FADI, FPFA
Dr. Mahoney was a member of the Dental Board of Australia's Committee on Sedation (2010-2020) and, panelled member of the Australian Health Practitioner Regulatory Agency (2010-2020). Greg was the president of the Australian Society of Dental Anaesthesiology (2009-2021) and the Australasian Military Medicine Association (20092019). Dr Mahoney presents courses and workshops for the Australian Dwntal Association and the dental industry lecturing in Australia, South East Asia, and Europe on the Local Anaesthetic including Local Anaesthetic Systemic Toxicity (LAST).

Reference List
1. Becker D, Reed K. Local Anesthetics: Review of Pharmacological Considerations. Anesth Prog. 2012;59(2):90- 102.
2. Peck TL. Hill SA. Pharmacology for Anaesthesia and Intensive Care. 4th Ed. Cambridge University Press. 2014. 4th ed. Cambridge University Press; 2014.
3. Kataria N, Jonnalagaddab S. Treatments, Mechanisms, and Adverse Reactions of Anesthetics and Analgesics, Chapter
16 - Prilocaine: Mechanisms and application. Academic Press; 2022.
4. Bryant B, Knights K. Pharmacology for health professionals. 3rd ed. Sydney: Mosby; 2011.
5. Drugbank. Drugbank. In: Retrieved from Drugbank Online [Internet]. 2023. Available from: https://go.drugbank.com/ drugs/DB00093
6. Navarro-Rodriguez J. Effectiveness of Topical Anesthetics in Pain Management for Dermal Injuries: A Systematic Review. J Clin Med. 2021;
7. Macfarlane A, Gitman M, Bornstein K, El-Boghdadly K, Weinberg G. Updates in our understanding of local
anaesthetic systemic toxicity: a narrative review. Anaesthesia. 2021;76:27-39.
8. Malamed S. Handbook of Local Aesthesia. 7th ed. St Louis: ELSERVIER; 2020.
9. Oertel R, Rahn R, Kirch W. Clinical Pharmacokinetics of Articaine. Clinical Pharmacokinetics. 1997;33:417-25.
10. Septodont MA. Submission Dossier for Septanest to FDA. Paris, France: Septodont; 2023.