
How to Create a Durable Bond to Zirconia
Zirconia is fast becoming the affordable aesthetic material of choice [1, 2]. The yttria-stabilised tetragonal zirconia polycrystals promote high mechanical strength and fracture resistance with optimal marginal fit to reduce microleakage [1, 3, 4]. Yet, many clinicians are challenged to achieve an optimal bond to Zirconia [3, 5]. This challenge can be overcome with novel material developments and advances in materials research and design [1, 5-7]. Here are five clinical tips to enhance your zirconia bonding, streamline your practice, improve your clinical outcomes and keep your patients happy.
1. Tooth preparation: Maximise restorative potential of zirconia.
To maximise zirconia strength and durability, opt for a digital impression following preparation [3]. Optimise the marginal fit by following an anatomical tooth preparation with 1-1.5 mm minimum reduction that includes a shoulder rather than a chamfer finish line with a cement space of 0.25-0.50 mm [3].
2. Pre-cementation: Prepare the tooth and restorative fitting surface.
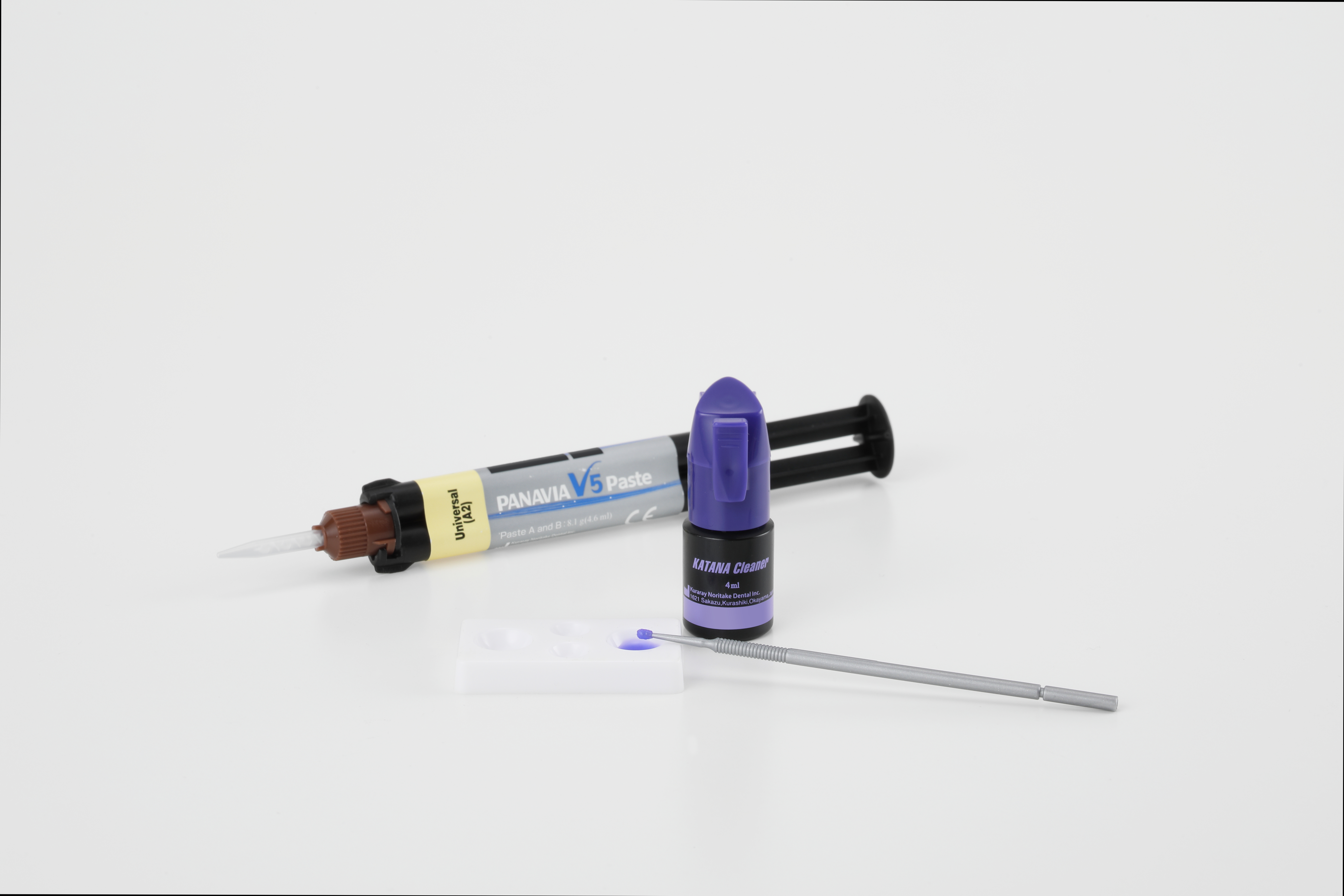
Use an ultrasonic scaler or pumice to remove temporary cement remnants from the teeth and zirconia restoration. Check the restoration fit and increase mechanical retention by air particle abrading the internal surface with aluminium oxide particles (50-60 mm alumina at 0.1-0.25 MPa or 14.5-36.25 psi for 15 seconds) [1, 2, 4, 5, 7]. Remove residue such as gypsum and try-in pastes from the prosthesis in an alcohol-soaked ultrasonic bath for 5 minutes [4, 5], or save time and enhance your bond by cleaning the fitting surface with a specialised abutment and fitting surface cleaner such as KATANA™ Cleaner (Kuraray Noritake Dental Inc.) [4, 8].
3. Isolate and decontaminate
Isolate your abutments from saliva, blood and moisture [1, 4, 5, 7]. Abrade the abutment surfaces to remove visible biological materials and contaminants. Select a surface cleaner [5, 7] such as KATANA™ Cleaner (Kuraray Noritake Dental Inc.), the only MDP salt formulation recommended for intra-oral use [9, 10].
4. Select a phosphate monomer-based cement.
Select an acidic functional phosphate monomer-based cement with the handling properties to suit your clinical situation and patient compliance [1, 4, 7]. Cements such as PANAVIA™ V5 and PANAVIA™ SA Cement Universal (Kuraray Noritake Dental Inc.) contain 10-MDP, the
manufacturer-prepared acidic functional phosphate monomer to form stable and durable [4, 11] chemical bonds between the metal oxides in the zirconia and tooth mineral [2, 7]. Two cement types you may consider include the dual-cured aesthetic, or self-curing cements to facilitate predictable bonding to zirconia.
Dual-cured aesthetic cements combine the benefits of shade matching with light and self-curing properties to increase working time and enhances practitioner control [2, 7] to allow for flexible curing in light-cure challenged intra-oral regions [4, 7]. Apply the dual-cured aesthetic cement, PANAVIA™ V5 (Kuraray Noritake Dental Inc.) , after treating the fitting surface with a silane and MDP-based CLEARFIL™ CERAMIC PRIMER PLUS (Kuraray Noritake Dental Inc.), and the tooth abutment with PANAVIA™ V5 Tooth Primer (Kuraray Noritake Dental Inc.) [2, 4] [2, 4, 5, 7].
If working time or aesthetics are less essential, a self-adhesive resin cement, PANAVIA™ SA Cement Universal (Kuraray Noritake Dental Inc.) may be the material of choice to adapt your restoration. You can enhance self-adhesive cement performance prostheses that lack retentive features by pre-treating [2, 4] the tooth surface with a MDP-based universal bonding agent such as CLEARFIL™ Universal Bond Quick 2 (Kuraray Noritake Dental Inc.) [5].
5. Follow instructions
Different products have unique application and curing requirements. To optimise results, follow the manufacturer’s instructions to maintain a strict thus predictable bonding protocol [1, 2, 4, 7].
In conclusion, to create durable zirconia bonds, adapt suitable tooth preparation, surface treatments, isolate from contaminants, select clinically appropriate adhesive materials and establish a manufacturer recommended protocol. Increase your satisfaction knowing that your newly acquired knowledge has potential to reduce post-operative sensitivity, increase restoration longevity, reduce warranty work to improve your long-term clinical outcomes, and keep you and your patients happy.

Dr. Arosha Weerakoon
BDSc (hons 1), PhD, MPH, FRACDS, FPFA, FICD
References
[1] Quigley NP, Loo DS, Choy C, Ha WN. Clinical efficacy of methods for bonding to zirconia: A systematic review. The Journal of Prosthetic Dentistry. 2021;125:231-40.
[2] Powers JM, O’Keefe KL. Guide to zirconia bonding essentials. New York, NY. 2009.
[3] Ahmed WM, Shariati B, Gazzaz AZ, Sayed ME, Carvalho RM. Fit of tooth-supported zirconia single crowns—A systematic review of the literature. Clinical and Experimental Dental Research. 2020;6:700-16. https://doi.org/10.1002/cre2.323
[4] Blatz MB, Conejo J, Alammar A, Ayub J. Current protocols for resin-bonded dental ceramics. Dental Clinics. 2022;66:603-25.
[5] O´ Connor C, Gavriil D. Predictable bonding of adhesive indirect restorations: factors for success. British Dental Journal. 2021;231:287-93.
[6] Comino-Garayoa R, Peláez J, Tobar C, Rodríguez V, Suárez MJ. Adhesion to zirconia: A systematic review of surface pretreatments and resin cements. Materials. 2021;14:2751.
[7] Blatz MB, Alammar A, Ayub JM, Rojas F, Conejo J. How to Bond to Current CAD/CAM Ceramics. Compendium of Continuing Education in Dentistry (15488578). 2023;44.
[8] Tajiri-Yamada Y, Mine A, Nakatani H, Kawaguchi-Uemura A, Matsumoto M, Hagino R, et al. MDP is effective for removing residual polycarboxylate temporary cement as an adhesion inhibitor. Dent Mater J. 2020;39:1087-95. 10.4012/dmj.2020-132
[9] Yazigi C, Kern M, Chaar MS. Comparison of bond strength to three restorative materials after contamination and the use of two cleaning agents. The Journal of Prosthetic Dentistry. 2023.
[10] Takahashi K, Yoshiyama T, Yokoyama A, Shimada Y, Yoshiyama M. Effect of decontamination materials on bond strength of saliva-contaminated CAD/CAM resin block and dentin. Dental materials journal. 2022;41:601-7.
[11] Yoshihara K, Nagaoka N, Okihara T, Kuroboshi M, Hayakawa S, Maruo Y, et al. Functional monomer impurity affects adhesive performance. Dental Materials. 2015;31:1493-501.